What do people know (that science/healthcare is undervaluing)?
People formerly known as patients (henceforth called people, see this post) know things about themselves and their context that professionals don’t know.
Pretty obvious, right?
While it’s obvious, the implications for health and healthcare are really important. Why?
As discussed in another post, evidence-based practice is a prevailing strategy used to guide clinical decision-making. Evidence-based practice uses “external evidence” from others, particularly insights from randomized controlled trials (RCTs), to determine what works “on average” for most people. Within this paradigm, acknowledgement that not everyone is “the average” is managed through the clinical expertise of clinicians. There is, of course, great wisdom to this approach as, between external evidence and clinical expertise, most individuals very likely receive the support they need in a cost-effective fashion that minimizes the need for a person to deeply understand their disease and health. This is particularly logical for acute diseases when, rightfully, a person wants support and an answer as quickly as possible.
As highlighted in that previous post, there is a third reference, which is a person’s self-knowledge, which is complementary information to the other two references but is currently undervalued, at a systems level, in evidence-based practice. For example, a recent study suggests that, when clinicians elicit a person’s agenda and insights about themselves, it takes, on average, 11 seconds before the clinician interrupts them. Clinicians are increasingly asked to do more in less time, and, thus, something often has to give. Unfortunately, often what gives is the time clinicians take to listen to patient priorities, experiences, and knowledge.
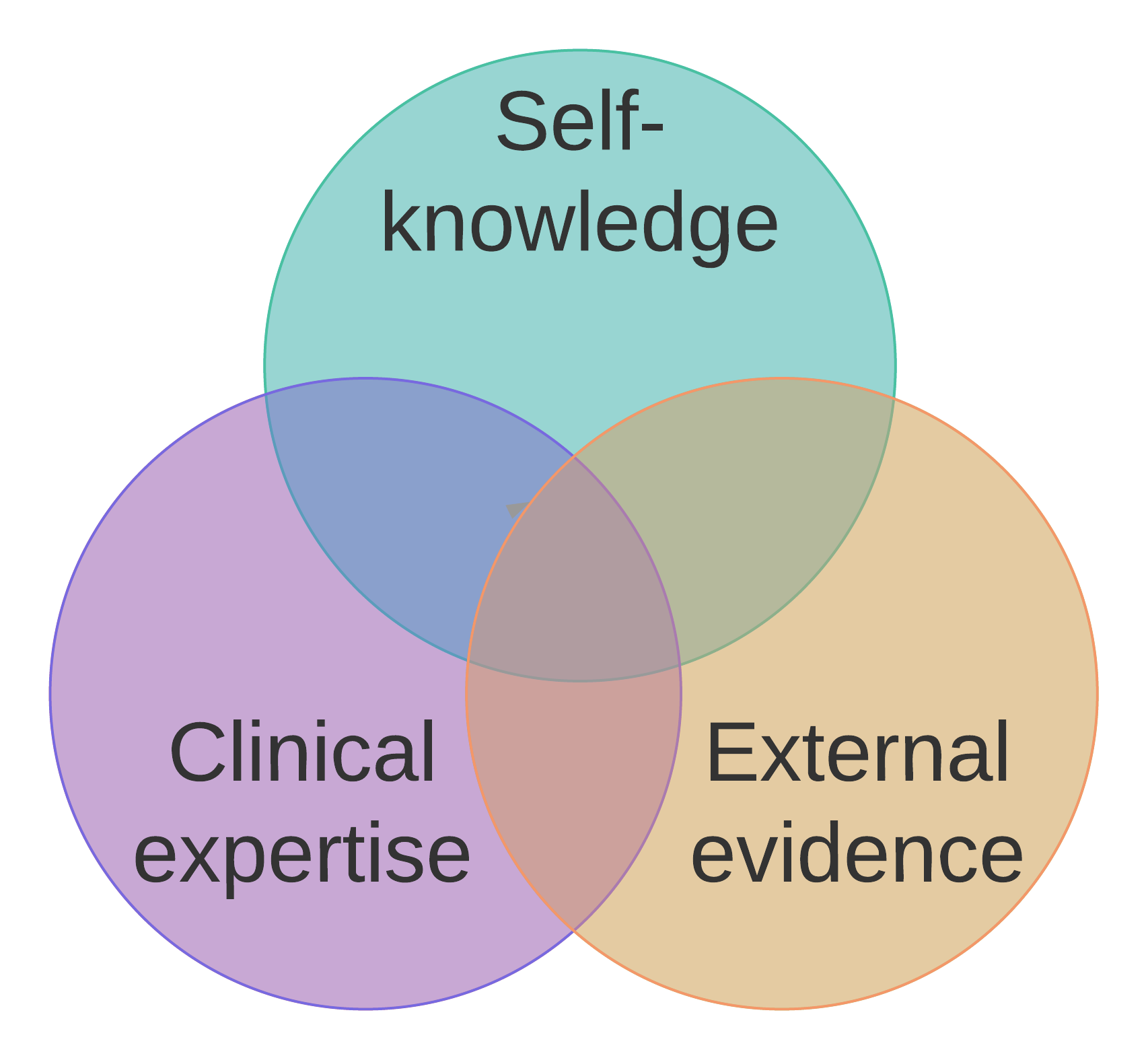
Arguably, a good clinical decision-making process would account for these three different forms of knowledge - self-knowledge, clinical expertise, and external evidence - particularly when in the realm of episodic and chronic conditions (see Figure; and, note, there are probably more, but for simplicity, we will focus on these three for now). While there is movement in the right direction for elevating this third reference to be more on balance with the other two (eg, precision health, PCORI, patient innovation), the overall structure of the health research and clinical practice enterprise systematically undervalues self-knowledge of people. As stated elsewhere, we strongly believe that researchers and clinicians are acting in good faith and doing the best they can to listen and engage with people. This is not a question of intent; it is a question of the overall system that makes it hard for self knowledge to be incorporated meaningfully.
When self knowledge in the form of individual differences and context are undervalued across the health research and clinical care enterprise relative to external evidence and clinical expertise, it creates problems across at least three levels:
- Clinically, it results in limited support for people who aren’t “the average.”
- Engineeringly, it results in undervaluing the insights individuals have about themselves and context when designing and engineering more robust solutions.
- Scientifically, it results in systematic undervaluing of context and individual differences in causal claims.
As is well known, the current healthcare system struggles with anyone who isn’t “the average patient.” If a person has a relatively “normal” profile for a given diagnostic state (e.g., a “normal diabetic”, inappropriate use of putting the disease first is being done explicitly; more in a moment), then the healthcare system does a great job. That’s because the external evidence and clinical experience are well-matched to this person. The clinician works through a series of diagnostic tools and rules to identify the “ballpark” of the person based on the external evidence, to identity the likely disease state(s) the person is experiencing. Once the clinician is “in the ballpark,” they can then take advantage of prior clinical experiences (expertise) to refine and ultimately finalize a diagnosis and make treatment recommendations. This, arguably works for most individuals (e.g., maybe 80 to 90% of individuals).
Before getting into the problems, its important to acknowledge the logic and elegance of this approach. If the insights needed for coming up with the right treatment are available in the external evidence and clinical expertise, then this is a highly efficient strategy for making decisions and providing support. This seems to be particularly true and valuable for acute care where, arguably, individual differences and context matter less, except in relation to exposures to various diseases. Indeed, the system, by design, will help most people without any requirement of the person to learn and know things, with the only requirement that the person trust the overall system and act in accordance with recommendations (though, as we’ve written elsewhere, there may be unintended consequences to this requirement). Further, as the series of steps highlight, it’s easy to see why both researchers producing external evidence and clinicians might fall into the trap of stating the disease state of a person first, prior to the person. Their job is primarily that of categorizing and clustering people to figure out useful strategies moving forward. While that doesn’t excuse the label, it does establish a logical reason for it, which could help to advance a solution (but that is for another post).
This process can run into problems if individual differences and context matter related to the person’s current health status. Why? Very likely it’s because some individual difference about the person (eg, genes, lifestyle, interaction between health conditions) or context (eg, exposures in the environment, socio-economic status, access to health promoting vs. compromising environments) are partially or fully driving a person’s overall health. While a good clinician can, feasibly, ask about this and incorporate it into their decision-making process, the time limitations of a clinic visit (eg, 15 minutes) make full transfer of this knowledge from a patient to a clinician hard and, thus, clinical expertise often is not fully accounting for these factors, particularly as they might impact a specific person’s health status. Put more simply, just how clinicians know things about disease states, treatments, and whatnot that people don’t know, people know some things about themselves and their context that professionals don’t know. Moving forward, the individual evidence pyramid provides a structure for clinical practice to incorporate self-knowledge, again, as a third reference that is complementary to external evidence and clinical expertise, to support and further refine support when a person falls outside of the boundaries of what is “known” based on external evidence and clinical expertise.
Ignoring individual differences and context sets up a huge loss for designing and engineering solutions to real-world problems. Why? Because context matters, particularly when a solution is implemented in the real world. This is being acknowledged in many circles. Human-centered design, as an approach, explicitly strives to understand meaningful differences in people and context to enable articulation of “design constraints” that one can use to increase the chances that a solution will be useful in real-world contexts. In implementation science “context is king,” is increasingly acknowledged. In behavioral design it is being called the “last mile problem.” Again, while progress is being made, systematically undervaluing self knowledge in the form of not including patients meaningfully in all stages of the process of creating and testing solutions to health problems hampers innovation.
Ignoring individual differences and context, is, unfortunately, a more systematic issue when we leave the clinical milieu or even the realm of design and engineering and move to scientific research, where the goal is to produce generalizable knowledge. Self knowledge is often either undervalued or, even worse, systematically ignored in the external evidence, and that’s really problematic from a causal standpoint.
In one of my classes, I teach students how to use self-experimentation and n-of-1 studies to try and improve their own lives. In brief, they work to study themselves to create their own solutions for producing some outcome they personally desire (eg, reduced stress, increased sleep, etc). My students present their results as a time series of data (eg, imagine a daily diagram of a person’s steps/day if they wanted to improve steps). Almost without fail, the student presenting results talks through the graph and identifies a few “outliers” on the graph, such as particularly high or low days. Almost always, the person has a pretty good hunch on what “caused” that outlier, such as ‘I visited the Grand Canyon and walked across it;’ ‘that was the day I had a wedding and so I ate a lot more than normal;’ or ‘that was the week before a really hard test.’ How reasonable are these “causal” claims? In my view, they are pretty darn reasonable as, if not the total cause, at least they play a partial role. Self knowledge helps a person to “see” that in data and it plays an important role in understanding, predicting, and ultimately controlling health outcomes for themselves as they can be more aware of the impact of context and idiosyncratic issues about themselves on those health outcomes.
What does a professional see in that same time series of data? An unexplainable outlier. What do they do? They manipulate the data to factor it out as if it’s not important or would somehow compromise the study. And, before it sounds like I’m blaming researchers, I want to highlight the logic and appropriateness of this. Researchers, by definition, don’t have the information they need to classify an outlier as anything but a statistical anomaly (outlier). As such, their hands are largely tied in using this strategy to enable them to still make progress on the other factors they are focusing on a plausible causal factors influencing an outcome of interest. Again, this is not a question of intent, it is a question on how the system and processes works to see if we can find better ways.
The result of this approach is that anything that impacts an outcome so strongly that it produces an outlier effect is systematically wiped out, averaged out, imputed, etc from the dataset. A central strategy for science to produce generalizable knowledge is via the articulation of robust causal models that define how something works. Based on this, this is a huge loss for the field, as arguably, some of the most influential causal factors of an outcome are systematically taken out of the data as standard practice. That could change greatly if self knowledge were accounted for more rigorously in scientific knowledge and information. This could be as simple as asking individuals to code their own outliers so that it could be factored into analyses (though we would need to find a way to do this in a low burden way) or establishing people formerly known as patients as essential members of a scientific team. Of course, individuals may be wrong about themselves, but at least this self knowledge can be incorporated into the data and, thus, the discussion for defining external evidence for future individuals.
In summary, people know things about themselves and their own context. The current processes professionals use are undervaluing these insights. A central goal of the Opening Pathways team is to integrate what people know into clinical care, engineering, and science as an important third reference alongside external evidence and clinical expertise as each reference provides unique insights that the other lacks.
